Faten khanfir1*, Mohamed Ali Hedhli1, Mohamed Tlili1, Mohamed Salah Khalfi1, Faten Ben Amor1
1.Université de Monastir, Faculté de médecine dentaire de Monastir, Laboratoire de recherche en santé orale et réhabilitation bucco-faciale, LR12ES11, 5000-Monastir (Tunisie)
*Correspondence: Faten khanfir, Male, Université de Monastir, Faculté de médecine dentaire de Monastir, Laboratoire de recherche en santé orale et réhabilitation bucco-faciale, LR12ES11, 5000-Monastir (Tunisie), Email: khanfirfaten@yahoo.fr
Received: 30 Sep, 2025; Accepted: 20 Oct, 2025; Published: 27 Oct, 2025.
Citation: Faten khanfir. Mohamed Ali Hedhli, Mohamed Tlili, Mohamed Salah Khalfi, and Faten Ben Amor. “Immediate guided implantation with aesthetic loading: a case report.” J Oral Dis Treat (2025):106. DOI: 10.59462/JODT.2.1.106
Copyright: © 2025 Faten khanfir. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribu tion, and reproduction in any medium, provided the original author and source are credited
Abstract
Introduction: This is a clinical case concerning the replacement of a maxillary left lateral incisor. Implant placement in the anterior sector represents a major aesthetic challenge for the dentist. Immediate implant placement with aesthetic loading is a reliable and effective protocol for rehabilitating one or more edentulous sectors. Guided surgery brings precision, safety, rapidity, and ease of access to the procedure. This advanced surgical approach, which is becoming increasingly popular, has been scientifically and clinically validated. Case report: This clinical case was about a patient in good general health who had suffered dental trauma to her 22. After a clinical and radiological examination, the decision was taken to place a 3.6 mm diameter, 12 mm high implant. This implant procedure was immediately followed by the aesthetic placement of an underbite PMMA resin provisional prosthesis on a temporary abutment.
Discussion: The guided immediate implantation approach with aesthetic placement meets the growing demand of patients seeking to minimize interventions and reduce treatment duration. However, it’s important to note that this technique should not be generalized, as managing failures is often more complex compared to conventional techniques. Therefore, the dentist must assess the case’s difficulty in relation to their experience, understand the indications and contraindications, and not exclude early or delayed implant placement. Conclusion: Immediate implant placement and aesthetic loading should be reserved for specific cases to ensure the success of these procedures, emphasizing the importance of a selective and careful approach in clinical decision-making.
Introduction
Implant-supported rehabilitation in the anterior sector represents one of the most delicate challenges in our field, requiring particular expertise.Aesthetic restoration and immediate implant extraction involves atraumatic extraction, followed by implant placement, and finally the creation of a temporary crown. This protocol offers significant advantages for both patient and practitioner, including psychological satisfaction, time savings and soft tissue management for optimal esthetic integration.
This protocol requires perfect knowledge of the anatomical structures visible on the different CBCT sections, which becomes more precise with the use of a digital surgical guide enabling the dentist to place the implant in the position of the future prosthesis already planned in advance.
Through a clinical case study, we highlight the importance of using a digital surgical guide for immediate implant placement. This case study highlights the many advantages inherent in this procedure, underlining its positive impact on clinical results.
Observssation
A 54-year-old female patient in good general health visited the outpatient department of the University Hospital Clinic of Odontology in Monastir, Tunisia, for therapeutic management of her left maxillary lateral incisor. Endo-buccal examination (Figure 1) revealed the presence of the 22 root
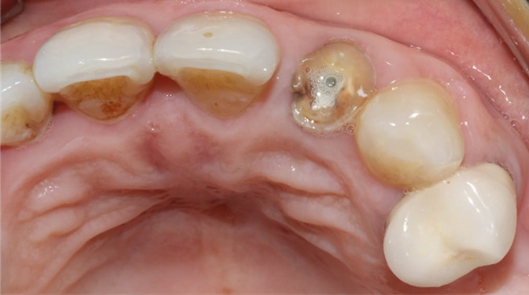
Figure 1. Occlusal view of the maxilla showing the fractured crown of the 22
Radiological examination (Figure 2) showed no periapical infection or desmodontal enlargement, and the presence of a thin layer of vestibular bone, so tooth 22 was deemed irrecoverable.
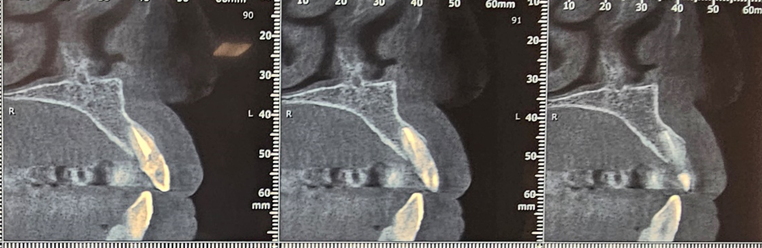
Figure 2. Sagittal sections of the CBCT of the patient
After discussing the treatment options with the patient, she opted for immediate implant-guided extraction with esthetic loading.
Operating Protocol
After scaling and root planing with hygiene motivation, we took a bimaxillary digital impression of the patient (Figure 3) and planned a tooth-supported surgical guide based on the complementarity between the STL file from the digital impression and the DICOM file from the CBCT (Figure 4, Figure 5).
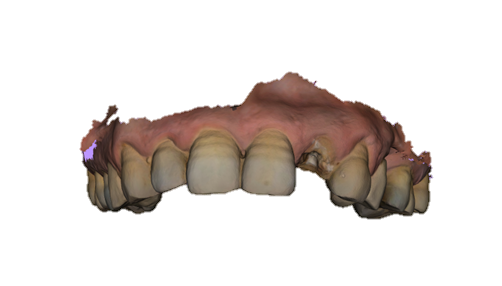 Figure 3. Maxillary impression with the 3Shape intraoral scanner
Figure 3. Maxillary impression with the 3Shape intraoral scanner
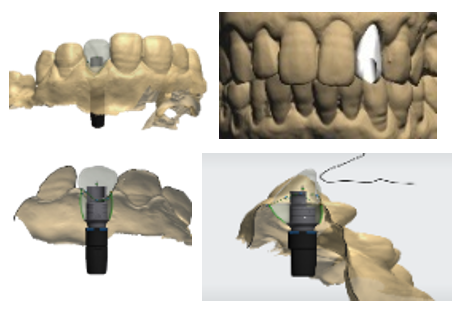
Figure 4. Modeling the provisional prosthesis and selecting the implant axis
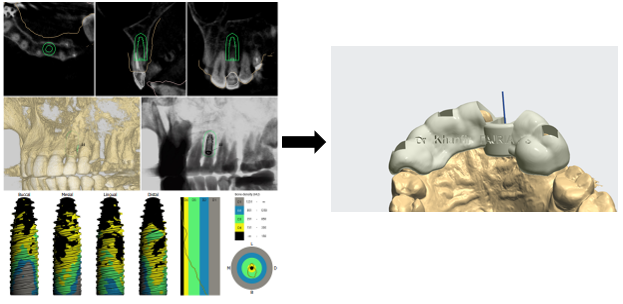
Figure 5. Combining STL and DICOM files to create a surgical guide
Surgical Phase
The patient presented for her third appointment for the surgical phase. We began by disinfecting the incisivo-canine region before administering local anaesthetic.
The 22 was then extracted atraumatically to preserve the bone on the vestibular side (Figure 6).
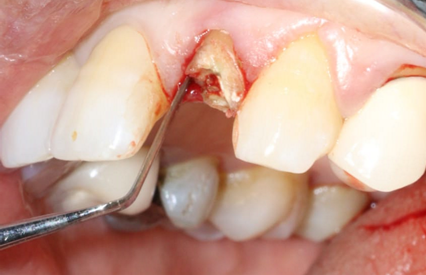 Figure 6. Atraumatic extraction of the 22
Figure 6. Atraumatic extraction of the 22
The surgical guide was placed and fixed (Figure 7) and we began the drilling sequence, to place a biotech 3,6/12 implant (Figure 8).
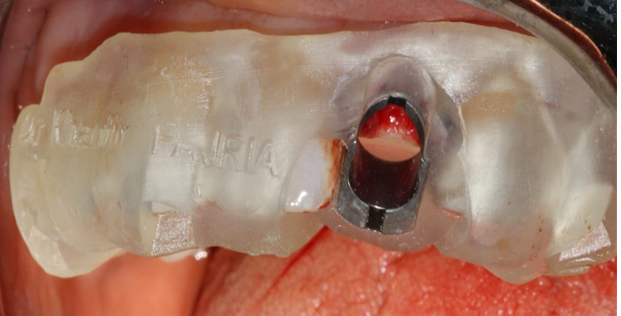 Figure 7. Placement of the surgical guide
Figure 7. Placement of the surgical guide
 Figure 8. Drilling sequence
Figure 8. Drilling sequence
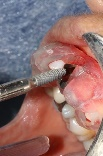 Figure 9. Implant placement
Figure 9. Implant placement
After implant placement (Figure 9), the primary stability of the implant was satisfactory (greater than 35N), the provisional abutment was fixed (Figure 10) and a post-operative retroalveolar radiograph was taken for radiological control of the implant and adaptation of the provisional abutment (Figure 11).
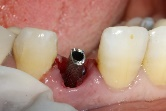 Figure 10. Fixing the temporary abutment to the implant />
Figure 10. Fixing the temporary abutment to the implant />
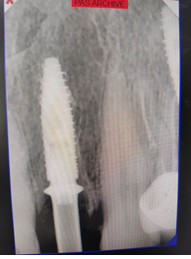 Figure 11. Postoperative retroalveolar radiography
Figure 11. Postoperative retroalveolar radiography
PMMA resin was placed around the provisional abutment, and the occlusion was checked to ensure that the provisional prosthesis was underbite (Figure12).
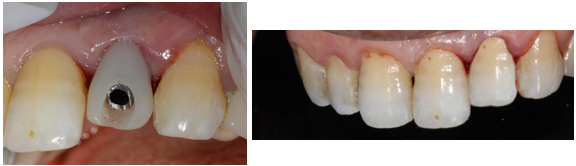 Figure 12. Placement of PMMA resin and final result of provisional prosthesis
Figure 12. Placement of PMMA resin and final result of provisional prosthesis
Prosthetic phase
After the 3-month period required for osseointegration of the implant, the patient was seen again (Figure 13) for a digital impression for the definitive prosthesis (using a scan body (Figure 14) and the fabrication of a Ti-base zirconia abutment (Figure 15), noting that the patient was under monthly clinical and radiological control.
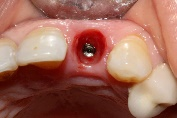 Figure 13. Occlusal view of gingival healing
Figure 13. Occlusal view of gingival healing
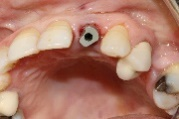 Figure 14. Occlusal view using the bodyscan
Figure 14. Occlusal view using the bodyscan
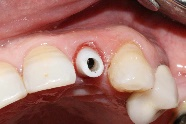 Figure 15. Occlusal view of Ti-base zirconia abutment
Figure 15. Occlusal view of Ti-base zirconia abutment
The crown was sealed and the patient is satisfied with her crown both aesthetically and functionally (Figure 16).
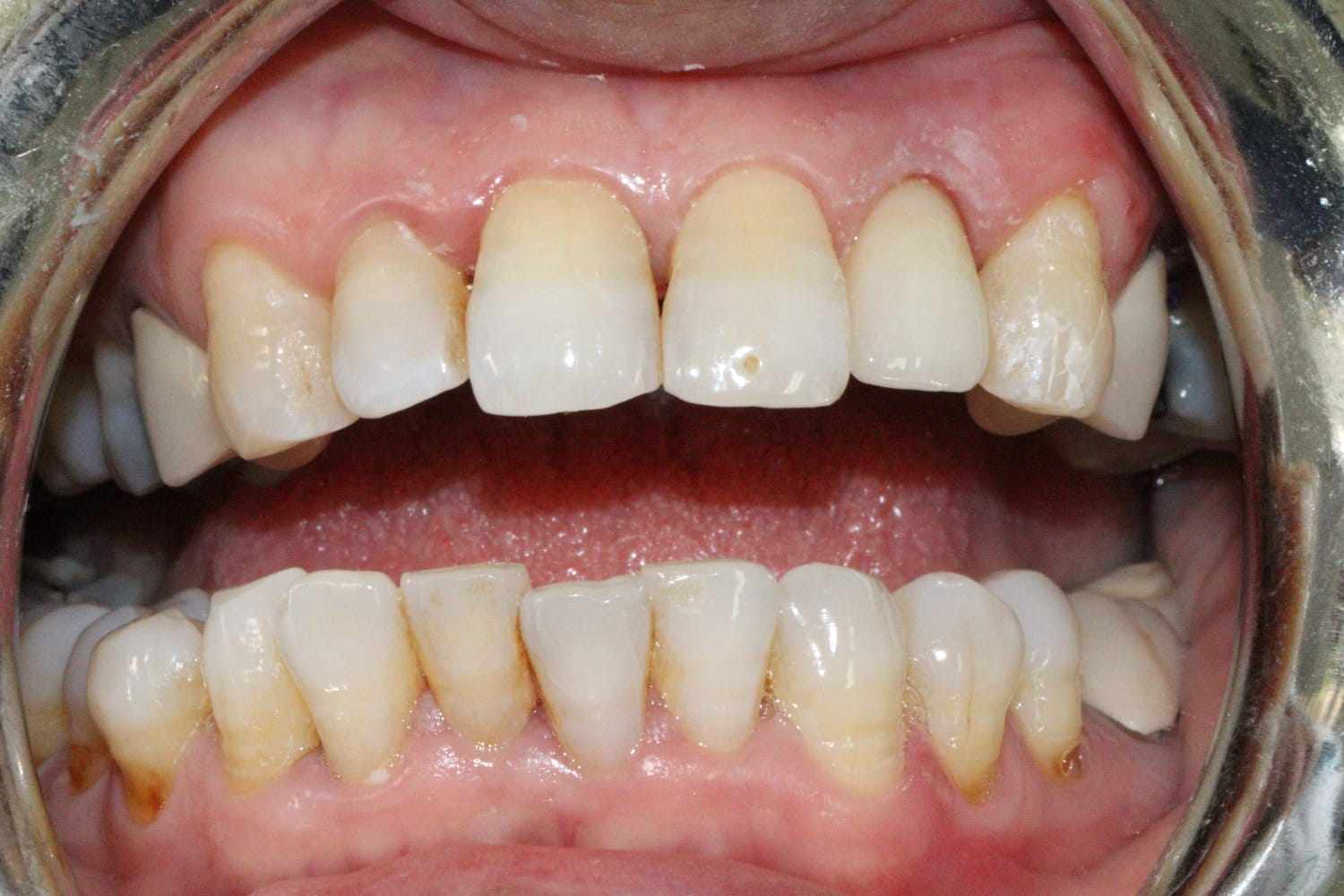 Figure 16. Sealing of the final prosthesis and final result of implant rehabilitation
Figure 16. Sealing of the final prosthesis and final result of implant rehabilitation
Discussion
Our clinical case represents an ideal example of immediate implant placement due to the presence of key indications for this technique, summarized as follows:
1. Intact Vestibular Bone Wall: Pre- and post extraction probing of the alveolar crest ensures identification of the vestibular cortical bone’s position, which is critical for determining the apico coronal placement of the implant. A minimum thickness of 1mm is required for successful outcomes. (2)
2. Favorable Mucogingival Environment: This includes the absence of asymmetries, perforations, or very thin tissues, which helps prevent infection risks and aesthetic complications. A minimum of 2mm of keratinized gingiva is recommended. (2)
3. Favorable Tooth and Residual Socket Anatomy: A minimum of three residual walls is necessary for success, as fewer than three walls increases the risk of failure. Moreover, an ectopic tooth position or a misalignment between the extraction and implant sites may render immediate replacement impossible. (3)
4. Sufficient Bone Volume: Adequate bone volume must be evaluated to ensure successful treatment. The integrity of the vestibular bone plate, the bone height beyond the tooth roots, and the presence of bone septa between adjacent teeth are critical for success. (1)
5. Absence of Acute Infection and Suppuration: According to literature, active infection and suppuration are considered contraindications for immediate implant placement. (4)
The guided immediate extraction-implantation method offers several benefits. It allows for a single, streamlined procedure without the need for a waiting period post-extraction, thereby eliminating multiple interventions and providing comfort during and after the operation, while also reducing stress and post-operative complications. (5) It also minimizes manipulation of the soft tissues and limits hard tissue resorption, a process that typically results in the loss of 40% of height and 60% of alveolar width within the first six months. This bone loss is exacerbated when the socket is damaged, such as by infection or the absence of a bone wall. This approach helps maintain adequate bone volume, which can be difficult to achieve after the usual healing period. (6)Additionally, extraction promotes a significant vascular supply due to the periodontal ligament and the opening of medullary spaces, which aids in the healing process. (7,8)
However, it is important to note that the application of this method is limited, and failure rates are higher when protocols are not strictly followed. Among the disadvantages are the high cost, the risk of aesthetic complications, and the uncertainty in outcomes due This technique requires precision in execution, and while it offers significant benefits, there is a margin of error. The accuracy of the 3D-printed surgical guide may vary between 0.25mm and 0.5mm, and the cone beam CT scan carries an error margin of around 0.6mm, giving a total error margin between 0.85mm and 1.1mm. (10,11)
Conclusion
Today, it is crucial to consider implantology from both an esthetic and a functional perspective. Patient expectations are evolving, as are techniques. What makes this approach particularly attractive is that the patient benefits from a new fixed tooth, offering an aesthetic result superior to that of a temporary removable prosthesis (12).
So, Thanks to advances in artificial intelligence and the use of a surgical guide, we are now able to treat complex cases, providing patients with less stressful and more comfortable care. However, clinical success depends on careful case selection. Immediate implant placement and esthetic loading should be reserved for specific patient profiles. The practitioner must assess the complexity of the case according to his or her experience, considering both early and delayed implant placement, without ruling out any possibility (9,12).
References